It’s pretty frustrating that masks became one of the biggest parts of the COVID culture wars.
As a result, it is really hard to talk about masks in a non-politicized way.
That’s unfortunate because it’s created a world where people have strong feelings on the effectiveness of masks despite very little evidence - and almost no high quality evidence - to tell us much about how well (or if) they work to protect us against the spread of SARS-CoV-2.
It’s one of the great scientific failures of the pandemic that we haven’t created the infrastructure to rigorously test out non-pharmacologic interventions in the United States.
As a consequence, for the past year and a half, we haven’t really fully understood how well masks (and mask mandates), ventilation, plastic barriers, and all of the other adaptations we’ve made to the pandemic actually work.
Almost a year ago, I wrote about the DANMASK-19 trial, which tried to measure the effectiveness of a mask mandate in Denmark. The study authors found that masks didn’t do all that much to prevent infection with COVID during the spring of 2020.
Caveats abound, of course, like that the total COVID numbers were low in Denmark during that time and more patients were lost to follow up than infected with COVID, but it was still curious. But one trial alone is almost never definitive.
That’s why the new trial on masks out of Bangladesh is so important.
The new mask trial is the highest quality trial of a nonpharmacologic intervention we have in COVID - and it can tell us a lot!
To start, I think it’s worth spending time on this study because it is the largest and most well done mask study that we have. It’s likely to be the most useful insight into the impact of masks that we get for some time (and maybe ever).
Carrying out this study was an amazing logistical feat. It’s an incredibly high quality study that I learned a ton from reading.
This was a cluster randomized trial - which means that rather than studying individual people randomly assigned to different treatment arms, they randomly assigned whole villages to different treatment arms. This method of study is particularly well suited to testing a difference in a method or approach to patient care (rather than investigating the impact of a specific medication or medical treatment).
In this study, they randomized 600 villages of people - that’s over 340,000 people! - to either cloth masks, surgical masks, or no masks at all.
For the groups assigned to masks, they gave people masks and promoted mask wearing. They also studied what made people more likely to wear masks (an interesting topic on its own that I won’t get into).
They planted people in the villages to directly observe mask wearing and they evaluated COVID infection via blood testing for evidence of infection.
The findings are really interesting. I’d like to point out a few of their results before we get into any discussion:
Mask wearing in the villages given masks was about 42% versus about 13% in the non-masked villages
Physical distancing also increased in the mask wearing groups, although by a smaller amount
The villages assigned to cloth masks did not have any reduction in COVID - this suggests that cloth masks are essentially worthless
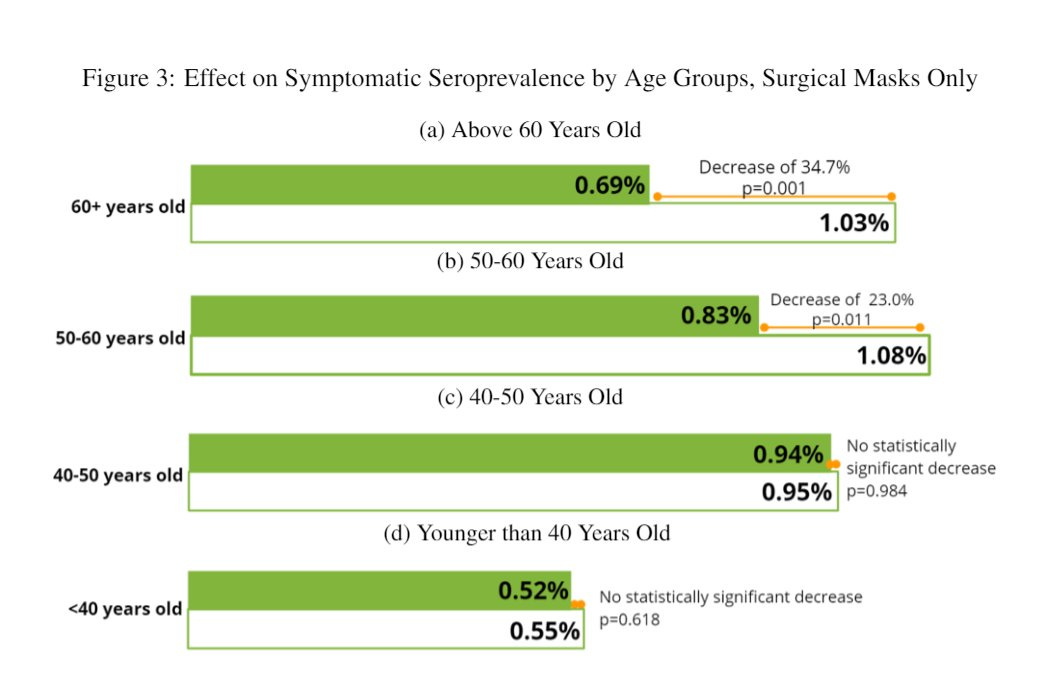
The villages assigned to surgical masks had a 12% reduction in COVID overall but the effect was really confined to older folks (over age 50):
We’ll come back to the age stratification in a bit, but first, let’s unpack some of those results.
Masks may be protective against community spread even if everyone isn’t wearing one
The researchers in this trial observed a decrease in spread of COVID with getting mask rates up from 13 to 42 percent.
So just getting an additional 29% of people to wear masks helped to cut down the overall community spread of COVID a non-trivial amount.
I suspect that this result is mostly driven by mask wearing itself with a small contribution from the increased physical distancing that was observed in masked folks (although it’s impossible to parse that out).
But if you had told me before that this is the difference in masking numbers that we would see during the trial, I would have predicted a neutral result. To see this size of an increase in mask wearing lead to a decrease in COVID spread is surprising to me.
When you start to think about viral spread as a multiplicative event, it certainly makes me a little bit more supportive of masking (especially if higher numbers can be achieved) than I was before this study.
Cloth masks probably don’t do anything
All of that work getting people to wear cloth face coverings for the past year and a half may have been pointless. There’s no signal in this trial - again, the largest and most important mask trial ever done - that cloth masks do anything.
So it’s possible that we’ve been wearing the wrong masks this whole time.
We should stop focusing efforts to get people to wear cloth face coverings. The evidence that they do much isn’t there, and when confronted with new evidence, it’s reasonable for us to change our minds.
Before this study, I thought cloth masks were reasonable, but that opinion has shifted after this trial.
Older people derive the most benefit from masking
We’ve all heard that age puts you at greater risk for COVID, and this study is no different.
It’s not really all that surprising that older people had the largest benefit here - they were measuring symptomatic infection confirmed with bloodwork. So it may be possible that younger people had a decrease in COVID infection with masking, but due to a lower incidence of symptoms, the benefit on symptomatic infection wasn’t seen.
TL;DR - what did you learn about masks from this study?
3 things:
Surgical masks - even worn by less than half the population - slow the spread of COVID
Cloth masks are probably pointless
Older people may be the only ones that see a benefit from masks. This is different than saying that older people are the only ones who should wear masks.
One other point about masks - the evidence on masking kids is very weak
Without belaboring the point - and certainly without getting into an argument about mask or vaccine mandates in school - I think it’s worth looking at some data on masking kids.
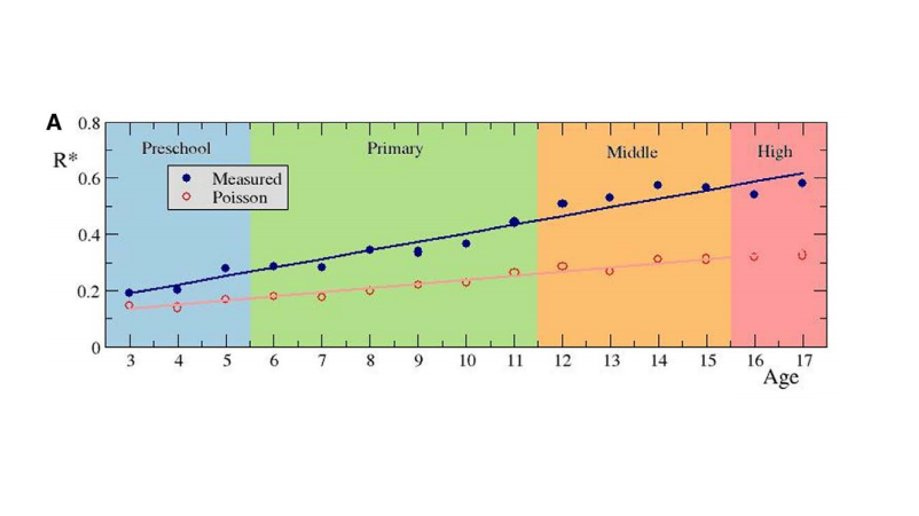
Look at this graph on kids wearing masks in Spain. The chart shows age on the horizontal axis, with infection rate on the vertical axis. Kids 5 and under didn’t wear masks and kids over 5 did wear masks:
What’s so fascinating about this graphic?
The lowest rate of transmission of COVID was in the group that wasn’t wearing masks! The curve suggests that age is the biggest predictor of risk, not masking status.
If masks made a difference for kids, you’d expect a jump up in the infection rate in the non-masked cohort, but instead we see the opposite.
Now, this isn’t a definitive trial and I would caution you from drawing any final conclusions, but it’s certainly intriguing data that would make me think twice before implementing a mask mandate in schools without stronger data to support my position.
And while we’re on the topic of masks and children, clearly the pandemic has made some of us go insane
Look at this article in the New York Times from an Associate Professor of Psychological and Brain sciences:
When I read this article, I thought that I was going crazy - on what planet do these arguments pass the smell test?
There are so many holes in the reasoning here, it’s not worth the time to go through them. But as a parent (and a human), I’m in shock that people find the idea that masks aren’t harmful to kids’ development to be plausible.
The absence of evidence is not evidence of absence.
And, as I think I’ve written before (quoting someone who I can’t remember but want to credit), SARS-CoV-2 is a virus that can affect any organ system that has an ACE-2 receptor in a patient, but only affects the brain of the treating physician and of policymakers.
Thank you for reading! Please share on social media and encourage your friends and family to subscribe!